
‘What works for you?’ Managing your medication
‘What works for you?’ Managing your medication
ADHD is rarely simple, it’s quite complex and defining how we treat something that is complex is the role of your clinician. And in simple terms this is where the expertise really lies, in treating ADHD properly.
At ADHD360 we pride ourselves on the standards of care we apply to working out what works to give you, our patient, the very best opportunity to achieve your potential.
We are often asked ‘how do you do this?’ and ‘what do I need to look out for?’ This 3T’s paper is focused on answering those and many more questions, and to help you understand what we mean when we say ‘we are titrating your medicine’.
There isn’t a one size fits all for ADHD medicine, there just isn’t. We need to understand this above all else as we start a treatment pathway.
There are four key stages to managing your medication:
Key Stage 1 – The focal points
Our clinicians have three main focal points, all aimed at helping you, those treatment focal points are:
- What other health considerations are there?
- What will success look like?
- What are your lifestyle need that we need to take into consideration
A comparison is probably the best way to discuss these three focal points.
Robert has recently got his first job, working in a factory.
He rides a moped to and from work and both he and his parents have asked that his treatment makes him safe to ride the moped in terms of his ADHD. His working day is 6am to 2pm and he sometimes has overtime to 6pm. His day therefore is at least 5.30am through to 2.45pm and often through to 6.45pm.
Robert is overweight, borderline at risk for diabetes and this needs to be considered.
William is at school, he is 9 years old and struggling to concentrate in class. Falling behind is frustrating him and he has all sorts of coping mechanisms for this but generally he wants to be able to ‘keep up’, not get frustrated and angry and to be happy.
He often loses his temper when he gets home from school, and his Mum and Dad bear the brunt of this frustration, which in the main he controls at school.
William is very slim, underweight for his height and this needs to be considered. He also has a diagnosis of Autism which is very relevant.
As you can see, they are two completely different sets of ‘needs’ and to treat them both the same would not give them both the success they want.
Key Stage 2 – Treatment requirements
Some medicines ‘kick in’ quickly, perhaps this is ideal for Robert as he gets up early. Some have a slow release mechanism that could help William, especially as some may last until he is home and with his family. If we compare the ‘highlights’ of ADHD medicines, you’ll see the complexity:
- Some ADHD medicines can last for 12 hours, some for less time, a few can last for 24 hours a day
- Some ADHD medicines take their time to ‘kick in’ when they are taken, some are immediate, but they may not last so long
- Some medicines have an immediate effect when you start treatment, some can take 7 weeks to be fully effective
- Some boost the medicine at key times of the day, some have a very steady and predictable release mechanism
Your clinician will take all of the three focal points into consideration, and then look at the medicines that are available before making a decision on what to try first. ‘Try first’ you may think? ‘What’s all this trying business, do you just not know right away? The simple answer is ‘no’ we don’t, and we can’t. Imagine a child with a broken arm, we can take an X-ray, a scan, have a look at the arm, and then decide what treatment is most relevant. We can’t see inside the brain so easily and the choice of medication is therefore more difficult.
Key Stage 3 – Choice of medicine group
Without over complicating things, we may need to boost the flow of particular chemicals in the brain such as dopamine, for some people we may need to improve the way the brain handles that flow, and each of these solutions may need different medication. There are three groups of ADHD medication, they work very differently and answer different problems:
- Amphetamine based medicine (stimulants)
- Methylphenidate based medicines (stimulants)
- Non-stimulant medicines
Your clinician will work with you to see which medicine group(s) work best for you; some people just don’t respond to one group, for instance they may not see any improvement using a methylphenidate based medicine, so we would ‘switch’ you to another group. We might switch you if you just don’t ‘get on’ with that medicine, we always pay great attention to any side effects. When we find the right group for you your clinician would then work on finding the right dose.
Here’s an interesting fact:
Some medicines are weight related, so that the heavier you are the more medicine you will need (that’s why we monitor your height and weight so much). Some drugs aren’t based on this, and the correct dose for a small, slight young man could be higher than the correct dose for a 5’10” female hockey player.
Key Stage 4 – The best dose
The big question now is ‘how does your clinician find out what the right dose is?’ Here’s the thing, it isn’t guess work, this is a process of monitoring and checking called ‘titration’. Your clinician will start you off a low dose of medicine and gradually increase this over time to see which dose works best for you. We have an iPhone app called ADHD360 which we often use to measure progress, have a look for it, it is free on the Apple App store.
Imagine you take your first dose of medicine, and bingo! You already see improvement. We had an email recently from a patient:
“This is amazing! I know it’s early days and I’ve only taken one tablet 3 hours ago but wow! I felt a wave go through my brain and I felt a bit weird and then it went, and it felt like a fog had been washed away! Is this normal? I also have loads of physical energy, but my mind feels calm.”
We could stop there, claim success, and settle for that medicine at that dose. Many clinics do.
But what if?
What if increasing the dose makes the fog go even farther away, makes her mind even calmer, for longer. We won’t know if we don’t try. So, we do try. And we persevere, titrating the medicine up slowly, checking to see where the peak of performance is, and checking this against any uncomfortable rise in side effects. We stay in touch, as a minimum every three weeks you have an appointment, sometimes more frequently, and we work with you to identify the most effective dose. We call this the ‘optimal dose’ and ‘optimising’ your treatment is our goal.
In Summary
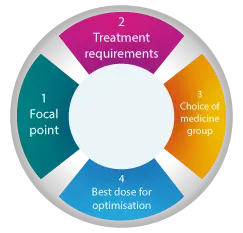
As a summary of all of this information there are four key stages for your clinician, and the more you understand these, the better it is for everyone as we medically treat your ADHD.
- Focal point
- Treatment requirements
- Choice of medicine group
- The best dose for optimisation
And that is why at ADHD360 we use the phrase ‘More than your diagnosis’ because treating you to the point where your symptoms are controlled to allow you to be the very best you can be, is more than a diagnosis.
In preparing this paper, ADHD360 acknowledges fully that medicine and medical treatment is just one option for the complete, holistic treatment of ADHD. Other papers will focus on alternative options and complementary interventions, such as coaching and counselling.
