
How do our clinicians get to be qualified as experts within ADHD360?
PASSION LED US HERE
How do our clinicians get to be qualified as experts within ADHD360?
When the Founders of ADHD360 sat together to work out just how we were going to make a new way of working actually function, we knew that we were going to disrupt the status quo and we had to ensure the very highest of standards if we were going to be visibly doing this. One area where we expected scrutiny was in the chosen workforce. This short 3T’s paper highlights our mindset and lets you, the reader, gain confidence in how your clinician is trained and monitored for competence throughout their career.

Background
In 2016, our Managing Director, Phil Anderton, was employed as a Management Consultant to work in NHS ADHD clinics looking for ways to make them more efficient and more effective. Efficiency can be viewed as how budgets are spent, staff utilised and how limited public funds are spent, whilst effectiveness can be seen as how the outcomes for the patients and staff were achieving standards, and indeed challenging if those standards were high enough to warrant being left unchecked going forward.
At this stage Phil had been working in and around ADHD for over 12 years, and had a CV that included working for PwC as a public sector management consultant, he was (and still is), heavily involved in the national ADHD advocacy charity ADDISS, and he was qualified as a project and programme manager as well as holding a Green Belt in lean 6 sigma, a process improvement and efficiency based international qualification.

Phil spent two years immersed in the NHS across the UK, working alongside clinicians and managers of all grades to ascertain what ‘excellence’ looked like. The ultimate goal was to find a service that completely represented excellence to use an example for others to model themselves on. Unfortunately, that goal was not satisfied, and what Phil did find was, sadly, a national picture that didnt always represent modern day requirements, perhaps commercially and financially not viable and in terms of processes, sometimes running inefficiently with wasteful ways of working. The landscape for the patient was not effective and long waiting lists, long gaps in treatment were common and many clinicians were unaware of the opportunities to ‘do better’ as this was, and generally still is, the ‘way we do it around here’.
Undaunted by the presence of mediocracy, Phil formed a small research team, with clinical representation, and continued to research what good / excellence would look like. The resulting paper, Pomegranate, was published to the national ABPI standards.
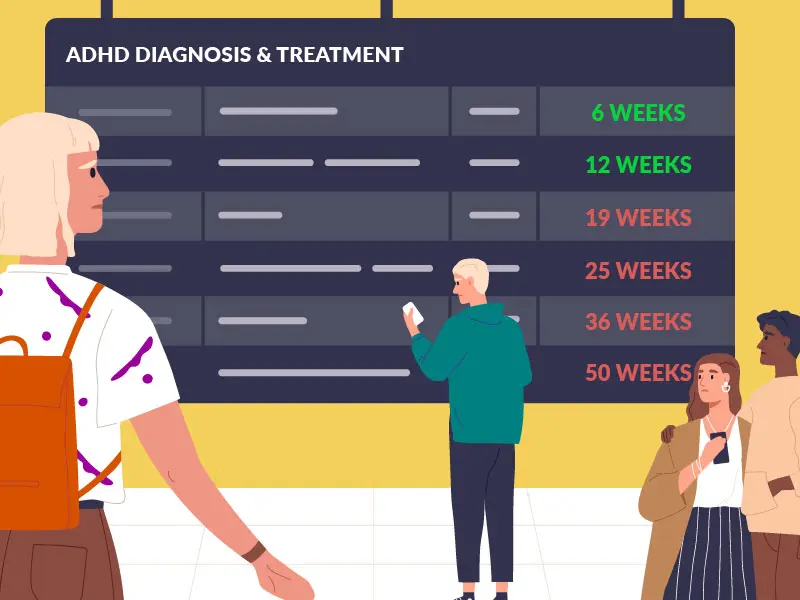
In this work, it was quite eye opening to find the mixed bag of standards across ADHD clinics. Some clinicians held no qualifications to work in ADHD, some assessment tools had been literally ‘made up’ by junior clinicians wanting to make a name for themselves by re-inventing the wheel, and in many cases, the processes being used were antiquated, outdated and wasteful of precious skills and resources. The inexcusable nature of this nationwide phenomenon should not be lost on anyone reading this paper.
Phil also found a 35 year waiting list in one area of England for adult ADHD assessments, and a Did Not Attend (DNA) rate of 70% that was not only being tolerated, it was being heralded as a ‘chance to catch my breath and have a break’ by a senior clinician leading that clinic.
All of this vital information became the basis for 360’s ways of working and we knew that we had to set the highest bar possible and change the ways things are done for ADHD across the UK. Not least of these challenges was the fact that clinicians needed to be upskilled and trained to far higher standards.
The NICE Guidelines, NG87

ADHD360’s Founders are privileged to have in the founding team, Jen Lewis-Neill, a highly experienced nurse practitioner that had sat on the small team that wrote and signed off the latest and current NICE guidelines for ADHD. NG87 itself changed things, reset the bar and challenged many, sadly not all, but many of the established ways of working within the ADHD community.
Jen is to this day an expert on national policy, the interpretation of the Guide and runs regular NG87 workshops for our teams.
At 1.3.1 NG87 states “A diagnosis of ADHD should only be made by a specialist psychiatrist, paediatrician or other appropriately qualified healthcare professional with training and expertise in the diagnosis of ADHD” The definition of an ‘appropriately qualified healthcare professional’ itself is nebulous and open to interpretation. Relying on Jen’s ‘inner knowledge’ we have taken the position that this includes the following:
- Any qualification MUST be underwritten by an appropriate national institution
- Any provider of the qualification MUST be suitably qualified to a national standard
- That the ‘healthcare professional’ does not have to include Consultant Psychiatrists and Paediatricians
Outdated thinking, still prevalent today, is that only a Consultant Psychiatrist or Paediatrician can assess and treat ADHD. This train of thought denies the very essence of NG87 that requires appropriate qualification, and we as a team acknowledged that a status in a medical hierarchy does not directly infer specialist knowledge. Throughout the research period mentioned above, the Pomegranate Years, many ‘specialists’ interviewed and shadowed in clinics were generalists and had very limited knowledge of ADHD, let alone the medications available for treatment.
In 2006 the NHS issued new professional guidance, focused on expanding the role of suitably competent nurses and pharmacists to become prescribers of medication. As non-medical prescribers (NMPs) this guidance gave authority for clinicians other than doctors to become more valuable and useful in clinical settings.
What was left for us therefore was to design a service that provided ‘appropriate qualification’ and fully utilised the essence of the 2006 report that stated at section 13 that organisations should “develop their strategic plan for the use of nonmedical prescribing to include independent prescribing by nurses and pharmacists.” That is exactly what we have done.
The operating model of ADHD360
Phil Anderton holds a Master’s Degree in Adult Education and training evaluation, and a PhD in workforce competency design, both from Hull University, handy given the 360 task!

The initial task was to accredit the organisation with a national body that held the credibility to satisfy the required compliance to ‘standard’. CPD UK was chosen, and ADHD360 is now an accredited training provider. The next step was to design and certify training programmes that would permit the appropriate use of the label ‘specialist’ in the field of ADHD assessment and treatment.
The Founders had looked at existing ‘leading’ programmes and found the standard to be set at a low bar, there was little available and what there was wouldn’t satisfy our requirements. Out of this the ADHD360 Academy was born. Now in its second year, the Academy is building a reputation of excellence and has trained over 70 clinicians, comprising of doctors, nurses and pharmacists.
But we recognised we needed ‘more’ to be able to truly satisfy that initial demand for the ‘highest standards’. The word ‘Preceptorship’ has been commonly used in medical circles for many years and its meaning of ‘a period of structured transition to guide and support all newly qualified practitioners from student to autonomous professional…’ as defined by the NHS seemed very appropriate for our next steps, and we set about designing the ADHD360 post Academy preceptorship programme.
There is an often-quoted Chinese phrase attributed to Xunzi:
“Not hearing is not as good as hearing. Hearing is not as good as seeing. Seeing is not as good as knowing. Knowing is not as good as acting. True learning continues until it is put into action”.
It is the essence of this statement that governs the next phase of our standards for becoming an appropriately qualified healthcare professional. Preceptorship for 360 focuses on ‘in action’ and will be repeated until deemed to have reached a satisfactory level. As this paper now details some of the nuances of preceptorship, we should be mindful that following this, there is one more vital step, that of maintenance and development of standards over time.
Preceptorship
Graduating from the Academy new recruits and potential recruits to 360 are placed on their Preceptorship programme. As they graduate, they will have already shadowed a full ADHD assessment and become aware of the prep’ for clinic process and the tools we use for assessment.
Initially, recruits will shadow at least one more if not two clinical ADHD assessments. The clinician they shadow will be a member of the clinical leadership team, a true expert in the field of ADHD assessment and treatment. Each of these shadow experiences is documented and debriefed and the candidate is tested for understanding of the process, the inputs and clinical outcomes. It is far from a ‘passive’ process.
Following shadowing the clinician is invited to assess a patient under close 1-2-1 supervision. The supervisor is again a member of the clinician leadership team and themselves trained in this process. The age of the patient is chosen to be relevant to the candidate’s own competence and professional skills.
The supervised session is tightly controlled. The supervisor in effect themselves assesses the patient, silently in the background and when the process is complete, and the treatment plan for the patient is formulated, the two clinicians exchange notes and views through a rigorous debrief process. Often at this stage, a clinician is ‘signed off’ as competent, but if either party doubts competence, other supervised sessions are arranged and monitored.

Post preceptorship final qualification
The 3-month probation period for every clinician joining 360 is an important next step on the journey to full competence. Only when ‘sign off’ of the probation occurs can we sit back and fully acknowledge the competence of the clinician as appropriate to our standards and requirements. Happily, we believe we set the bar far higher than the ‘norm’.
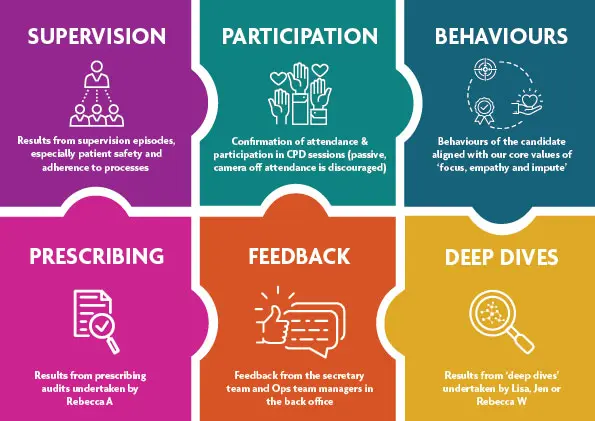
Probationary clinicians are scrutinised according to our 6 common clinical standards, known as our 6 Categories of Clinical Excellence (6 CCE’s). The 6 CCE’s are:
- Supervision, performed regularly including sessions by an external Key Opinion Leader in national and international ADHD clinical standards
- Participation in regular training sessions, more than mere attendance
- Behaviours against the 360 core values
- Prescribing standards, through weekly quality checks and daily standards audit
- Feedback from front office staff, clinical team leaders, our Quality Assurance team and patients through Trustpilot
- ‘Deep dives’ – a process where 6 random patient files are scrutinised to a very deep level by a specially trained clinical manager.
The 6 CCE form the bedrock of all on-going assessments for clinicians and together with other tools, they are the foundation for all our clinical standards.

Overall
ADHD360 believe we have the highest of standards for our clinical work. We recognise that we cannot possibly satisfy everyone all of the time, but we try our very best and we have a robust, standardised process for accrediting our clinical team, that is not only compliant with current guidance but sets the ‘bar’ far higher than anything we found during the ‘Pomegranate’ years and through our considerable years of experience in the ADHD360 environments, both here in the UK and abroad.
