
Why it is important to think below the neck when treating ADHD
“ADHD can reduce life expectancy by as much as 13 years, but this risk is reversible.” (Russell Barkley, 2022).
This is a shocking headline, and as we examine it, we see the importance of drawing attention to the continued risk and vulnerabilities for people with ADHD. The risks aren’t what you would think they may be. To start, let’s look at what the statement refers to.
The obvious and first question is: why is this statement made?
The discussion should centre around reassurance, the concern of ‘if I have ADHD I am going to die?’ Reading this headline could induce anxiety, if not mild hysteria. It shouldn’t. The many studies on this subject are purposeful and designed to attract the attention of policy makers and service commissioners. If the headlines read ‘there is no risk of ADHD and premature ageing’ there would probably be even more inattention to the need for more investment in ADHD services.
So be reassured that a diagnosis of ADHD does not automatically lead to premature death. However, and there is always a ‘but’, there are many additional risk factors for a shortened lifespan that patients with ADHD should acknowledge and deal with effectively. In the context of providing a service, such as those offered by ADHD360, the staff and clinical teams of the service should be ‘all over’ these risks. The service should be working with the patient to mitigate them, reducing them to the lowest impact possible.

ADHD as a deficiency of dopamine in the prefrontal cortex is not the cause of the alarming statement at the beginning of this paper. However, the associated risks of poorly managed ADHD are the genesis of the concerns and relevant risk-based discussions.
At a conference in Autumn 2023 in Colorado, Professor Rakesh Jain asked the esteemed audience why the life expectancy for people with schizophrenia is shorter than those without. Was it suicide? Was it depression? No, he answered, it was heart disease. This is also the case with ADHD, as well as a few other preventable health matters.
Correlation between ADHD and other illnesses
Adverse health and lifestyle factors are the main contributors, together with self-regulation and deficits in planning skills that place an additional burden on the patient and then flow over into life expectancy. But what are those lifestyle factors? And what is meant by adverse health factors?
Let’s examine the statement made by Professor Jain about the significance of heart disease and the cross over to ADHD.
People with ADHD have a chronic illness, it is pervasive and impactful. The well documented deficits in executive functioning (EF) caused by ADHD give rise to a series of life events that when put together as a set of actions and consequences, begin to build the ‘story’.
Diet
It takes planning to have a healthy diet. What to eat has to be carefully considered, as does when to eat it. When to purchase ingredients is also an important factor. Additionally, we can supplement this list of tasks with the actual process of cooking a meal and maybe even following a recipe. It isn’t difficult to see where on that list the person with poorly managed or untreated ADHD may struggle. There are also many drop off points where failure will completely close out the task. The alternatives would rarely be cited by a nutritionist as a ‘healthy’ option.

The benefits of a personalised eating / management plan are well documented, protein is important and avoiding many food groups that are unhelpful to the person with ADHD. Ned Helliwell, the much-published clinician from the USA, recommends that the plate for a person with ADHD should be half fruit or vegetables, a quarter with protein, and the remaining quarter only with carbs.
As the discussion continues, we can hopefully see how difficult it is to plan healthy eating, execute it, and enjoy the eating process when we are laden with all of these executive function challenges.
Addictive behaviours
I am frequently asked to discuss the links between addiction and ADHD. Some 20 years ago, back in 2004, I attended a conference session about ADHD and addiction. I expected a lot of rhetoric about cocaine and heroin, which was covered, but more importantly, the overall general risks of addiction were discussed at length.
The ADHD brain has a deficit of known chemicals in the relevant parts of the prefrontal cortex. That much is commonly known and understood. When we delve deeper, we learn that if we supply a ‘fix’ to that chemical imbalance, it’s pleasurable. That feeling of pleasure releases hormones of its own, and that euphoric sensation becomes addictive.
The ‘fix’ could be running or hard exercise. For some it may be playing a challenging game on a console. For many - far too many - it is the use of substances that are harmful to our health that are frequented, and then addictively pursued.
As people sit in judgement about these matters, it is fundamentally important to understand that for the person with untreated or poorly managed ADHD, this may well not be a matter of individual choice to experiment and take harmful drugs. Being poorly drives behaviours, and these are more often than not, choice based decisions.
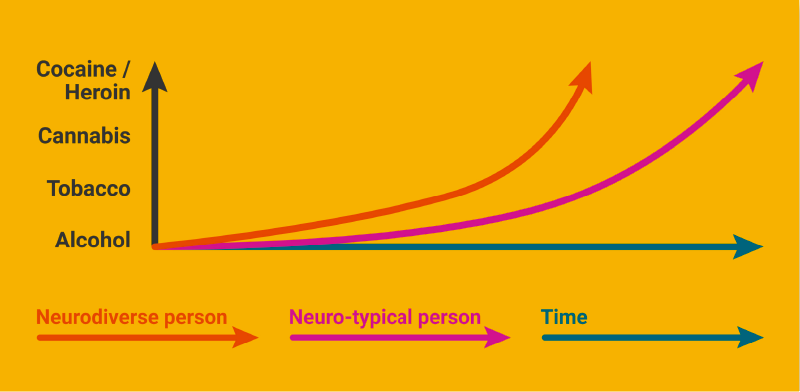
The pathway through substances is well charted and written about by such ADHD legends as Dr Tim Willens, who as an American MD specialises in Adolescent Psychiatry and Substance Abuse Services. Willens cites that the journey through harmful substances is more rapid for people with ADHD than neuro-typical subjects and the move from interest and experimentation to clinical addiction is also accelerated.
ADHD360's 'Below the Neck' Approach
Substance Abuse and ADHD
Drugs
When interviewing drug addicts with ADHD the pathway was clearly demonstrated and evidenced:
“I used to get drunk to level off my mind and slow things down, but that was obviously not sustainable, so I switched to cannabis - itself visible and easily smelt - then to cocaine which has an amazing calming effect and is harder for people to see.”
“When all my mates take cocaine they get high, when I take it, I can sit down and watch Coronation Street for the first time. It’s like I can concentrate like normal people.”
Sadly, what they are experiencing is by definition, self medication of their ADHD symptoms to overcome their chemical deficits. This generates feelings of relief and pleasure, which - as we know - become addictive. Perhaps those who seek to challenge treating ADHD with appropriate medication should be comparing the risks to not taking medication and having a homespun regime to fill the gaps, which is far riskier than managing the side effects of those medications.
Nicotine
Of course, we need to examine nicotine and tobacco use. Smoking causes cancer, heart disease, stroke and lung disease. Every year 76,000 people die in the UK from smoking, with many more living with debilitating smoking related illnesses (NHS, 2022). There is a huge agenda across the NHS and social care to reduce smoking - but not many of those funded schemes actually look for a cause of smoking rather than simply recognising it as a choice.
This was once described to me as:
We are getting quite good at pulling drowning people out of the stream, but we aren’t good at all at working out how they fell in!
Here’s the science: Studies suggest that the alpha-4 beta-2 nicotinic acetylcholine receptor is the main receptor that mediates nicotine dependence. Nicotine acts on those receptors to facilitate neurotransmitter release of dopamine producing pleasure and mood modulation. I directly link this to the needs of the untreated, or poorly treated ADHD brain. It’s addictive. It’s dangerous.
Pulling all of this together for a healthier, and longer life
What we have looked at so far is the obvious - and yes, it may read as obvious - but there is a long way to go across families and healthcare providers to move the obvious ‘common sense’ into ‘common practice’.
To do this we have to challenge conventional wisdom.
This presents us with an issue. You see, conventional opinion regarding ADHD is like concrete; it hardens and you can then do nothing with it.
We seem to have an approach to getting more help for ADHD, no matter what the issue, we seem to rely on changes in conventional NHS commissioners’ thinking, but it’s set like reinforced concrete.

The time is right to approach getting more for people with ADHD in a different way.
Imagine approaching your GP or your child’s school teacher, and that they are resistant to the whole ‘ADHD thing. Imagine asking for help with a weight gain problem, obesity, smoking, drinking alcohol, smoking, poor diet, and making the case that:
- I am at increased risk of heart disease
- I need to lose weight and have a healthy BMI
- I need to reduce my chances of having a stroke by quitting smoking
- I need to stop taking cocaine to get through the working day
- I need to seriously eat healthier, but I can’t work it all out
To do this, will you please screen me (or my child) for ADHD? Screening for ADHD takes minutes, literally only minutes.
What next?
We are often exposed to more concrete thinking.
The NHS cannot afford to assess and treat the thousands of people who have ADHD.
The costs of modern medicines for ADHD are prohibitive.
We should examine the alternatives:
- Smoking has cost the NHS £2.6 billion a year!
- Smoking costs GPs across England £1.1 billion a year, and they act as the first port of call
- 50% of life-long smokers die prematurely, losing on average about 10 years of their life (Gov.uk)
- Government spending on smoking cessation programme is at a record high of £138 million (Gov.uk)
- The cost of people in the UK being overweight is £98 billion and the direct cost to the NHS is £19.2 billion, described as a public health disaster (The Guardian)
- According to NHS England in 2021, 26% of adults in the UK are obese
- £25,000 is spent, every minute, on diabetes in the UK, totalling £14 billion a year
- Assessing and treating a person for ADHD, including medication costs is about £2,500 a year
There are 67 million people in the UK. We should accept that 5% will have ADHD, so that’s a total possible ADHD population of about 3.3 million people. It would cost about £6.5 billion to treat everyone properly for their ADHD. That’s a lot of cash, however, even if we only stack this up against the cost of treating smoking and diabetes, never mind alcohol and drug abuse, we have a potential saving of £10 billion.

For many reasons, we have to understand the overall health implications of ADHD, especially ‘below the neck’.
It is accepted that the equations used to make this argument are simplistic, but they are also impactful.
It is not just the prerogative and responsibility of policy makers to effect change, it is the role of anyone connected to ADHD to seek to make a difference, whether that is for yourself, your family or those you serve through your role.
The hidden impact of ADHD on the wider public health agenda has to be exposed, and it may, just may, bring about a breakdown in concrete thinking and allow us to pull our loved ones out the streams they keep falling into.
If you are struggling to get help from your GP, or your school for suspected ADHD, look wider, look below the neck and build a separate and different compelling case for change.
If you have ADHD or suspect you do, or you are the parent of someone possibly with ADHD, look to help them with diet, weight gain, smoking, etc. These are all risk factors for a shorter, unhealthier life, and this can be prevented.
Start your journey
Sign up today and start your ADHD diagnosis and treatment journey